
Deviation of the ST-segment (elevation or depression compared to the isoelectric line) can be a sign of ischemia of the heart muscle. In most of individuals without prior cardiac disease, the ST segment is at the level of the preceding P-R segment and/or the following T-P segment (so called isoelectric). Further, the elderly, patients of female gender, and diabetic patients frequently present with symptoms that are not typical, further emphasizing the role of the presenting ECG for diagnosis and triage of such individuals. Although the innovation of cardiac troponin (cTn) assays specific to the myocardium is changing the overall diagnosis of MI, the decision to proceed with angiography or give thrombolytics is made based on STE on the ECG and is usually reached before troponins are detectable in the blood. By these guidelines, pPCI is recommended for those with symptoms indicative of ischemia of the heart muscle that began 12 h or less before medical encounter who have elevation of the ST segment. In contrast, the guidelines recommend initial conservative therapy for patients with suspected MI without STE, as active ongoing ischemia may not be present and earlier studies have not shown a benefit for reperfusion therapy in patients without STE.Īs per the 2013 ACCF/AHA Guideline for the Management of ST-Elevation Myocardial Infarction, ST elevation myocardial infarction is a clinical syndrome that compromizes typical symptoms of acute ischemia of the heart muscle in conjunction with elevation of the ST segment and increased blood levels of biomarkers that indicate necrosis of the cardiac muscle. Therefore, it is recommended that patients with suspected acute STEMI and without contraindications should be subjected as soon as possible to therapy intended to recanalize the occluded artery by either primary percutaneous coronary intervention (pPCI) or fibrinolysis. ST elevation (STE) is considered to reflect acute transmural ischemia caused by an occlusion of an epicardial coronary artery by a blood clot. 
Additionally, serial ECGs every 15 to 30 min should be performed in patients with ongoing symptoms in whom the initial ECG is not diagnostic of ST elevation MI (STEMI). Per the “Third Universal Definition of Myocardial Infarction” document, the ECG should be acquired and interpreted within 10 min of presentation. Today, the electrocardiogram (ECG) is the most commonly used diagnostic tool for recognizing and triaging of patients with symptoms suggestive of myocardial infarction (MI). In writing this paper, we hope for quicker and better stratification of patients with STE on ECG, which will lead to be better outcomes. Here, we present the different patterns of non-ischemic STE and methods of distinguishing between them. 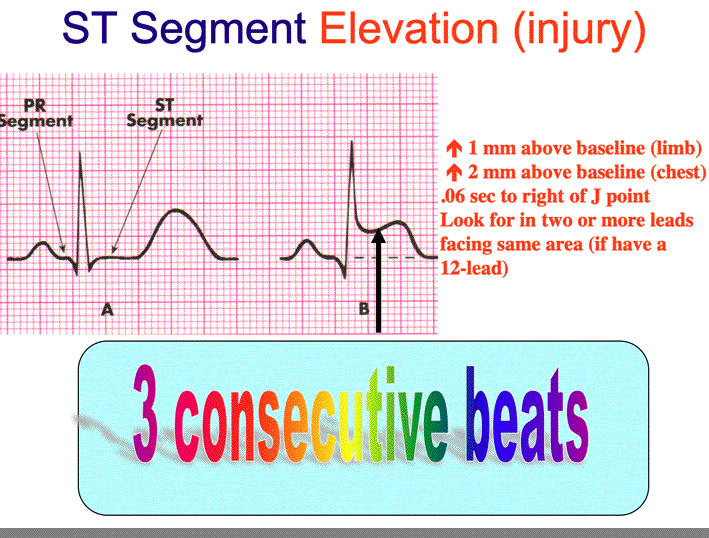
No matter the strategy, at the heart of delivering the best care lies rapid and accurate interpretation of the ECG. Multiples strategies have been tested and studied, and are currently being further perfected. But its importance cannot be ignored, as reflected in the 2013 American College of Cardiology Foundation/American Heart Association guidelines concerning the treatment of ST elevation myocardial infarction. Coordination of interpreting the ECG in its clinical context and appropriately activating the pPCI protocol has proved a difficult task in borderline cases. 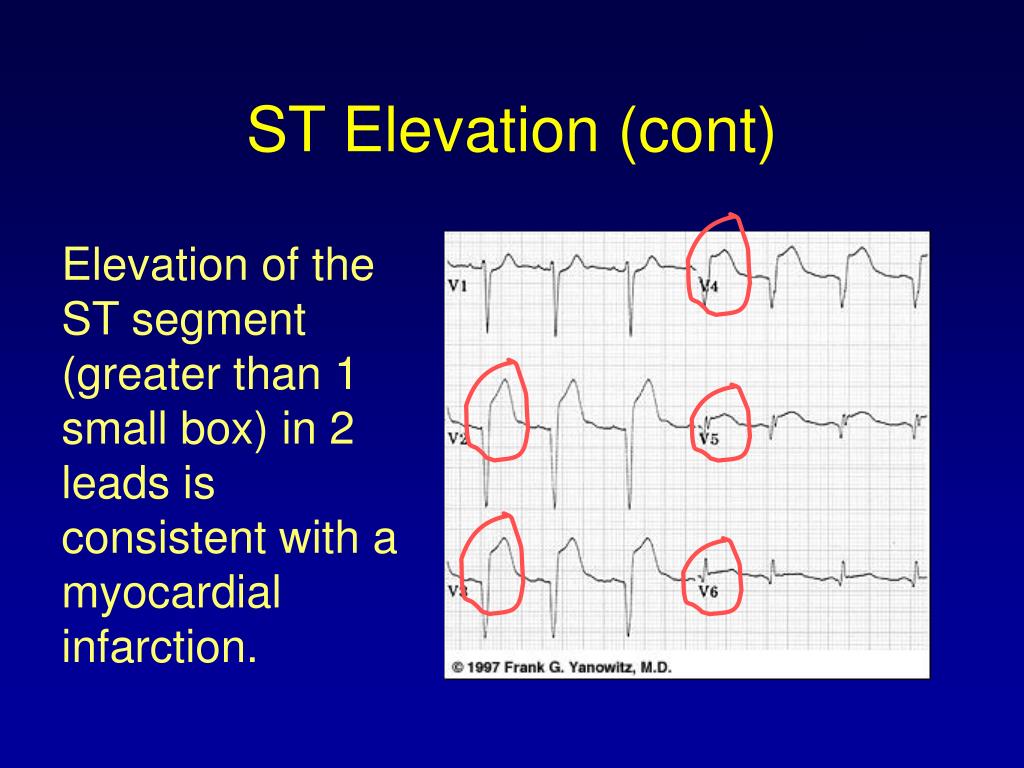
As a result, activating the primary percutaneous coronary intervention (pPCI) protocol often depends on determining which ST elevation patterns reflect transmural infarction due to acute coronary artery thrombosis. Non-ischemic STE may be confused as STEMI, but can also mask STEMI on electrocardiogram (ECG). In addition, ST elevation (STE) caused by conditions other than acute ischemia is common. The benefits of early perfusion in ST elevation myocardial infarctions (STEMI) are established however, early perfusion of non-ST elevation myocardial infarctions has not been shown to be beneficial.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
